| Research Article | ||
Open Vet. J.. 2025; 15(2): 863-870 Open Veterinary Journal, (2025), Vol. 15(2): 863-870 Research Article Use of 3D printed low-cost models for veterinary clinical skills trainingNedžad Hadžiomerović1*, Amila Šunje-Rizvan2, Alan Maksimović2, Lejla Šatrović3 and Faruk Tandir11Department of Basic Sciences of Veterinary Medicine, Veterinary Faculty, University of Sarajevo, Sarajevo, Bosnia and Herzegovina 2Department of Clinical Sciences of Veterinary Medicine, Veterinary Faculty, University of Sarajevo, Sarajevo, Bosnia and Herzegovina 3Department of Veterinary Public Health and Legislation, Veterinary Faculty, University of Sarajevo, Sarajevo, Bosnia and Herzegovina *Corresponding Author: Nedžad Hadžiomerović. Department of Basic Sciences of Veterinary Medicine, University of Sarajevo–Veterinary Faculty, Sarajevo, Bosnia and Herzegovina. Email: nedzad.hadziomerovic [at] vfs.unsa.ba Submitted: 13/11/2024 Accepted: 23/01/2025 Published: 28/02/2025 © 2025 Open Veterinary Journal
AbstractBackground: Three-dimensional printing is used in veterinary medicine to produce precise physical models for education, research, and training. As simulation-based approaches in veterinary education continually improve, we are exploring the applicability of three dimensional (3D) printing technology for this purpose. Aim: The aim of this study was to evaluate the level of student satisfaction, motivation, and confidence with the introduction of 3D-printed models in veterinary clinical training. Methods: A total of 57 students from the University of Sarajevo–Veterinary Faculty were included in the study. The groups were created according to the previous clinical training: third-year students with dominant observational and little active participation, fourth-year students with modest active participation, and fifth-year students with high prominent active participation in the clinical work. The students attended the theoretical review and practical presentation prior to their work on 3D printing models. Upon completion of the activity, students were given a survey that included questions divided into four categories: general satisfaction, comparison with traditional teaching methods, interactivity and practical application, and technical characteristics. Results: Students exhibited a positive attitude toward the use of the three dimensional printing (3DP) models as clinical simulators. This innovative approach could reduce stress when transitioning to work with live animals while enhancing interest in clinical work. Conclusion: The significant benefits of the 3DP include enhanced durability, low production costs, and a significant reduction in the number of cadavers needed for educational purposes. Keywords: Additive manufacturing, Clinical skills, Simulation, Veterinary education. Introduction3D printing is a technique that uses 3D CAD datasets to create physical objects. It is also referred to as additive manufacturing, and it has the primary advantage of fabricating almost any complex shape or geometric feature (Rengier et al., 2010). The use of 3D printing for medical purposes started in the early 2000s and rapidly increased across various domains of medical education and practice (Leukers et al., 2005). An important factor contributing to this trend was the transformation from very expensive to accessible and affordable 3D printing technology (Griffey, 2014). In veterinary medicine, 3D printing is used to create precise anatomical models for education, training, and research (Kapoor, 2024). The fused deposition modeling (FDM) printing technology is most commonly used, especially for making 3D models for education and research, allowing rapid prototyping and printing of large objects (Wilhite and Wölfel, 2019). Physical 3D models enable students to identify complex anatomical structures and understand their spatial relationships. Learning and practicing clinical skills on 3D models offers multiple benefits: improved animal welfare, reduced student anxiety, reduced use of cadavers, standardized and timely learning, and the ability to perfect skills through repeated practice without ethical concerns (Langebæk et al., 2012; Fredieu et al., 2015). Additionally, the significant advantages include low production costs, durable materials, easy storage, and models that are both reusable and replicable (Hadžiomerović et al., 2023; Cheo et al., 2024). The educational value of three dimensional printing (3DP) models has been extensively examined in various studies. These investigations have consistently revealed that students perceive the 3DP models as highly effective tools, particularly in terms of enhancing performance, promoting long-term knowledge retention, and increasing both motivation and satisfaction (Chedid et al., 2020; O’Brien et al., 2021; Hammerton et al., 2022). Acquiring clinical skills and applying theoretical knowledge in veterinary education is always challenging due to the lack of patients and ethical concerns. Thus, precise anatomical models are vital in educational and training settings across all stages of veterinary education, including undergraduate and postgraduate programs, clinical skills training, and client education (Yilgör Huri̇ and Oto, 2022). Technological improvement has become very popular, allowing more interactive learning in comparison with traditional medical education. Recently, many veterinary schools have introduced simulation labs in their curricula to provide better clinical skills for students, which is a key aspect of their work. Introducing simulation-based training allows students to gain experience as an artificial representation of a real-life process to achieve educational goals through experiential learning (Al-Elq, 2010). With the growing demand for training and the limited availability of animals and cadavers, we utilized 3D-printed technology to prepare cost-effective models for clinical practice. The aim of this study was to evaluate the level of student satisfaction, motivation, and confidence using 3D-printed models in veterinary clinical training. Materials and MethodsStudy designPrior to working with the 3DP models, students were given a theoretical review and practical presentation about the upcoming work. Four clinical models were introduced: a canine front limb for vein cannulation, an antebrachium with a paw for bandaging practice, a canine head for dental regional anesthesia, and a canine pelvis and spine for epidural anesthesia. The cannulation model included an anatomical model for regional anatomy review, and the canine head model was paired with a feline head model to highlight the anatomical differences between the species (Figs. 1–3). Upon completion of the activity, students were given a survey that included 17 questions that were measured using a 5-point Likert scale.
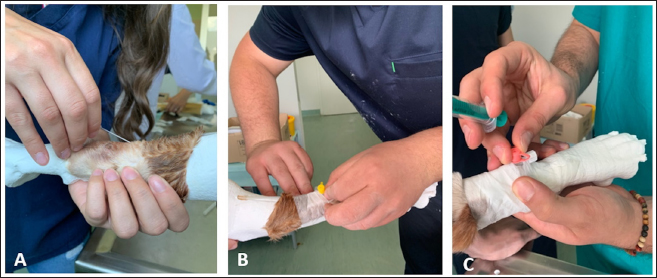
Fig. 1. Students working in groups of two using models to practice intravenous catheterization. One student restrained the model, stabilized the limb and raised the vein. The other student is performing intravenous (IV) catheter placement (A), secure taping (B), and flushing with saline (C).
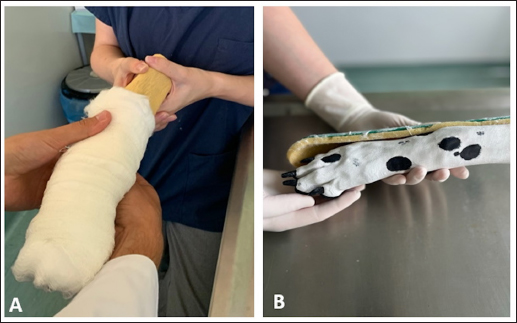
Fig. 2. Students working in groups of two using models to practice bandaging technique. One student manipulating the model and the other bandaging the limb. Bandaging of the wounds (A) and splinting (B) was performed.
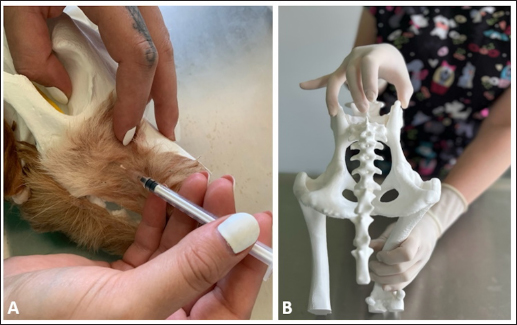
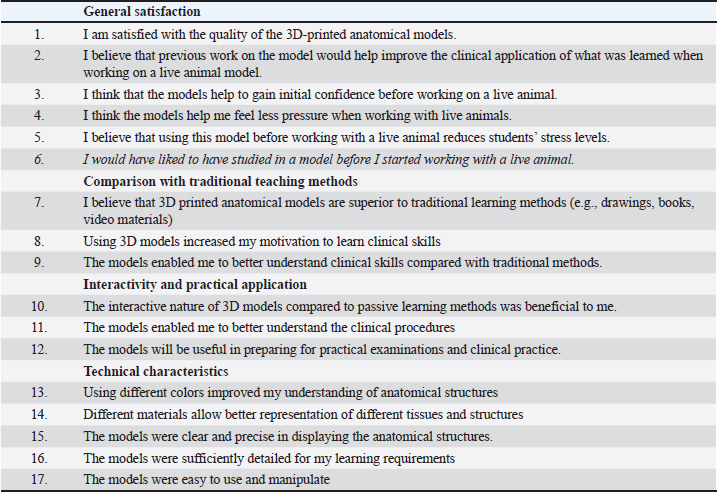
Fig. 3. Students working in small groups using models to practice regional nerve blocks for dental and oral surgery (A) and epidural anesthesia of the dog (B). The questions were divided into four categories: general satisfaction, comparison with traditional teaching methods, interactivity and practical application, and technical characteristics. A single question was reserved for students who had already worked with live animals; therefore, it has not been answered by all participants (Q6). The survey also included a section for student feedback with space for comments, suggestions for improvement, and ideas for future models. Design and 3D printing of modelsThe FDM printing technology was used to produce 3D printed models for clinical simulation. This technology is based on the extrusion of material (filament) transferred through a preheated nozzle and the creation of a layer-by-layer product structure on a print bed. A wide range of materials can be used with FDM printers; the most common is polylactic acid (PLA). Although PLA showed less resistant and flexible than thermoplastic polyurethane in bone printing (Kurt et al., 2022), PLA was selected for its advantages in terms of reduced printing time and lower material costs. The datasets were obtained in different file formats (CT/ magnetic resonance imaging (MRI) or 3D models) from online sources like thingverse.com or sketchfab.com. The best-quality 3D datasets are usually obtained from the computed tomography (CT) because the scan resolution ranges from 0.625 to 0.10 mm. A different file format was transferred to .stl printing format, and with the slicer Cura 5.6.0, a 3D model was prepared for 3D printing. A slicer converts a 3D model into a set of instructions (G-code) that a 3D printer can use for 3D printing. The “normal” printing parameters were selected in the Cura slicer, and most of the models were printed in the vertical printing orientation with a “tree” support structure using the Ultimaker S3 printer. The support structures were removed after printing, and the final phase included the preparation and painting of the models. ParticipantsA total of 57 third, fourth, and fifth-year students from the University of Sarajevo–Veterinary Faculty were included in the study. Their participation was voluntary. Regarding previous clinical training, third-year (n=31), fourth-year (n=19), and fifth-year (n=7) students had low (observational with little active participation), moderate (observational with modest active participation), and high (observational with prominent active participation) levels of clinical skills, respectively. Most of the higher-year students had hands-on experience with live animals, but none of the participating students had worked with 3D-printed models before. Thus, three groups with different levels of clinical experience and skills were formed. Specific demographic information about the students participating in this activity was not collected to preserve the anonymity of the study participants, and an informed consent form was obtained from all the students. The inclusion criteria for the study required participants to have attended both the theoretical review and practical presentation on the use of 3DP models in veterinary clinical training, as well as previous clinical training sessions at the veterinary faculty. The exclusion criteria were participants who had not attended the practical presentation on 3D printed models or who did not provide consent to participate in the survey. Statistical analysisAn analysis of variance was conducted to examine statistical differences among the study groups. The mean values and standard deviations of the students’ responses were calculated and are presented in Table 2. Statistical analyses were performed using the SPSS software package (SPSS for Windows, Version 22.0). Table 1. Survey on the level of student satisfaction with 3DP models.
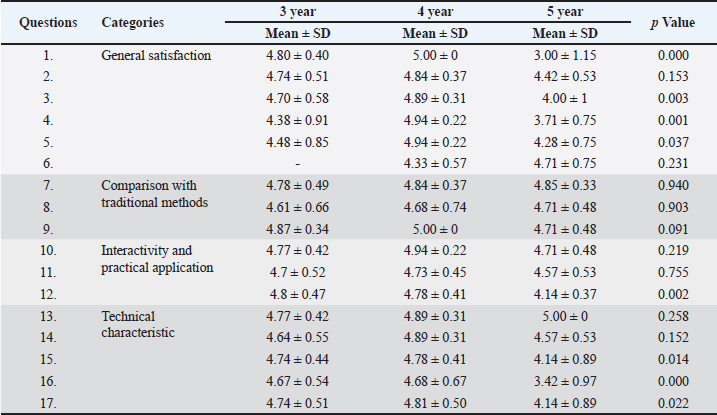
Table 2. Student responses reflecting attitudes toward the use of 3DP models.
ResultsThis study was conducted in 2024 with a sample of 57 students who were offered to answer questions related to their general satisfaction with the use of the 3DP models (questions 1–6), their comparison with traditional teaching methods (questions 7–9), interactivity and practical application (questions 10–12), and technical characteristics (questions 13–17). Regarding the category of general satisfaction, fourth-year students reported the highest level of satisfaction with the quality of the 3D printed anatomical models (likert scale mean ± SD=5.0 ± 0). The satisfaction level was also statistically significantly higher compared with the fifth-year students (3.00 ± 1.15). Comparison with traditional teaching methods did not notably differ between groups of students. The attitudes of the fourth and fifth-year students differed in relation to the Interactivity and practical application category, specifically, their opinions that the previous work on the models would lead to better application of what was learned while working on live animals (4.84 ± 0.37, 4.42 ± 0.53, respectively) and that the models would help to gain preliminary confidence before working on a live animal (4.89 ± 0.31, 4.0 ± 1.0, fourth- and fifth-year students, respectively). The most common student feedback was that innovative teaching methods enhanced their interest in clinical work. “I believe that this method of learning is much more efficient, primarily because of gaining experience in working with models. Also, it is much more interesting and easier to remember this type of lessons”. “I think it is an excellent idea. 3D models will help students and make me more interested in practical clinical works”. The use of the 3DP model could reduce stress in subsequent work with live animals (4.94 ± 0.22, fourth year), allowing the animals to feel less pressure during real clinical work. However, significant differences were observed in the pressure and stress levels experienced by students before working with live animals, with fifth-year students reporting mean values of 3.71 and 4.28, respectively). The fifth-year students emphasized that they would like to practice using models before starting to work on live animals (4.71 ± 0.75). “3D models should be included in the preclinical subjects, for better understanding of the study content and preparation for work in clinical subjects”. Participants with scarce clinical experiences, the third-year students, also agreed about the quality of the created 3D printed anatomical models (4.80 ± 0.40), but they showed more agreement than the fifth-year students in connection with the statement about preliminary confidence before working on a live animal (4.70 ± 0.58). All groups preferred using 3D models over traditional learning methods, and students gave more preference to the applicability of 3D models in contrast to drawings, books, videos, and other traditional learning methods (mean range=4.78–4.85), whereby fifth-year students mostly agreed that the use of 3D models increased their motivation to learn clinical skills (4.71 ± 0.48). In this section, this question got the most uniformly dispersed; students of all included years strongly agreed that the models gave them a better understanding of clinical skills compared to traditional ones. The highest degree of opinion was found in questions that assessed students’ attitudes toward interactivity and the practical application of the 3DP models. All surveyed students highly agreed that the interactive application of the models benefits them (third year: 4.77 ± 0.42, fourth year: 4,94 ± 0.22, fifth year: 4,71 ± 0.48) as well as that the models enable them to better understand clinical procedures (third year: 4.70 ± 0.52, fourth year: 4.73 ± 0.45, fifth year: 4.57 ± 0.53). Most students expressed satisfaction with the models and offered suggestions for future improvements. “In addition to the currently offered cannulation models, I would supplement with a model of the hind leg. A model for practicing blocks used in equine models would also be very useful”. Reflecting on the technical characteristics of the models, third- and fourth-year students overwhelmingly agreed that the use of different colors on the models significantly enhanced their understanding of anatomical structures (4.77 ± 0.42 and 4.89 ± 0.31, respectively). Notably, fifth-year students demonstrated complete uniformity in their responses, rating the effectiveness of colored models at 5.0 ± 0. Discussion3D printing technology has been used in veterinary medicine to produce precise anatomical models of bones and organs, serving as valuable tools for education, training, and research. Previous studies have investigated and compared the usability and effectiveness of 3D-printed models for learning anatomy. Superior results were recorded when comparing 3D printed cardiac, gastrocolic, and brain models to 2D images, traditional cardiac models, and formalin-fixed brain specimens (Wang et al., 2017; Chen et al., 2020; Hadžiomerović et al., 2023). The 3D-printed models of the ovine stomach were extremely useful for enhancing spatial understanding and illustrating the topographical relationships with neighboring anatomical structures (Mendaza-De Cal and Royo, 2021). In a veterinary curriculum, acquiring clinical skills is one of the most important components, but it is also quite challenging due to ethical concerns associated with practicing on live animals. The use of simulation technology can provide artificial representations for training, enhancing student experience while preserving patient safety (Issenberg et al., 2005). The incorporation of simulators into veterinary education is a relatively recent and innovative area of study. These tools provide a safe, controlled, and repeatable environment for students to practice clinical procedures while ensuring ethical considerations. Although simulators cannot completely replace the use of live animals for instruction, they offer a valuable opportunity for students to hone their skills before working with live patients. These teaching simulators enable the development of practical skills without the need for a live patient, leading to more confident graduates with enhanced proficiency in practical skills. Simulation-based medical education enriches the learning environment and provides substantial educational benefits by supporting the development of technical skills and clinical competencies among veterinary students. In addition, it serves as a valuable solution to address the challenges posed by limited faculty and staff resources in training programs (Casimir et al., 2022). A very important aspect of simulators is that they contribute to animal welfare by reducing reliance on live animals in educational settings (Scalese et al., 2005; Baillie 2007). An important aspect of simulation training is reducing the stress that students experience when performing surgery on live animals (Altwal et al., 2022). Research conducted by Edinburgh University demonstrated that repeated exposure to low-fidelity surgical training models increased final-year students’ surgical confidence and competence and reduced procedural stress related to three key surgical entrustable professional activities (EPAs) (Thompson et al., 2023). The use of low-fidelity models, such as table-top simulators, offers valuable alternatives because of their low cost, ease of construction, and ability to effectively meet teaching objectives. A key advantage of these models is that they provide multiple opportunities for learners to practice and repeat technical skills as often as necessary to achieve competency (Perez-Rivero et al., 2022). A review article (Braid, 2022) researching four databases (CAB Abstracts, Scopus, ScienceDirect, and Wiley Online Library) on the use of simulators for teaching practical clinical skills to veterinary students concluded that practicing on models produced learning outcomes that match or surpass those achieved through cadaver or live animal sessions. Using simulators during training can increase students’ confidence in task performance and in recognizing anatomical structures or landmarks, even if their ability to perform the actual task does not improve. In addition, simulators help alleviate student anxiety before conducting procedures on live animals. Therefore, the results of our research are consistent with the findings of similar studies and indicate that veterinary students at the University of Sarajevo greatly benefit from the use of simulators in clinical practice classes when it comes to acquiring clinical skills and lowering the stress and pressure when performing the learned skills on the live animal. The most experienced fifth-year students had the opportunity to compare work on 3D models and live patients, and they confirmed that they would prefer working on models prior to working on live animals. However, in certain aspects, such as the quality and details of the models and the reduction of pressure levels, fifth-year students reported lower values. This is understandable given their level of knowledge and prior experience working with live animals. Studies (Erickson, 2019; Pohl et al., 2022; Marsch et al., 2024; Neubauer et al., 2024) have shown that veterinary medicine is a stressful field and one of the most stressful occupations. That’s why lowering the stress in the teaching environment and having more confident graduates are important for the mental health of future veterinarians. The 3D printed models are commonly used to teach anatomy to first-year students and as simulation models for internal medicine and surgery. A study by Diaz-Reganon et al. (2024) evaluated the perceptions of first-year and fifth-year students regarding their learning experience with an upper endoscopy model based on 3D printing technology. The prepared model, featuring realistic size, texture, color, and appearance, along with detailed inner surfaces including gastric folds and a pyloric sphincter, was highly regarded by the students. Both student groups perceived the 3DP as an effective learning tool. For anatomy students, it served as a valuable supplement without completely replacing real specimens. In contrast, fifth-year students were more enthusiastic and regarded the model as an essential tool for clinical training. A variety of veterinary simulation models for small animals are available on the market from various companies. The most common types are leg vascular access models, intubation models, canine neuter simulations, and suture pads. These models are often made using flexible and replaceable materials, and their prices typically range from $500 to $1000 USD. The frequent use of these models incurs additional costs for replacement parts. Producing printed plastic models requires an initial investment in a 3D printer, with prices varying depending on the model, ranging from $500 to $3,000 USD. The material cost for each of our models does not exceed $10 USD, with an extra charge for painting services. In addition, multiple copies can be easily and rapidly printed from a single prepared model. The overall cost of preparing 3D printed models is significantly lower than that of using cadavers or purchased simulation models. Previous studies have regarded PLA as the most available, cheap, easy-to-use, and durable material for the 3D printing of educational models (Cojocaru et al., 2022; Ekim et al., 2024). This study examined the use of 3D-printed models in veterinary clinical training and their impact on students’ confidence and motivation using a simulation-based approach. However, several limitations of this study should be acknowledged. First, the sample size was relatively small, comprising 57 students, and the analysis was limited to immediate feedback following the use of the 3DP models, without examining their long-term impact on students’ clinical skills, knowledge retention, or confidence in real-world scenarios. A comprehensive understanding could be achieved by evaluating students’ performance and comparing their outcomes with those obtained through traditional teaching methods. Future research should include a more controlled experimental design to directly compare the effectiveness of 3DP models with conventional teaching approaches, focusing on various dimensions such as knowledge retention, skill acquisition, and practical application in clinical environments. Additionally, incorporating feedback from educators and clinicians who have implemented the 3DP models in their teaching practices would provide valuable insights into the feasibility, effectiveness, and challenges of using these models in real-world educational contexts. Expanding the scope of the study to include a broader range of simulation models and analyzing their relative effectiveness across different teaching methodologies would also contribute to a deeper understanding of their pedagogical value. ConclusionThe research findings propose the utilization of 3D-printed anatomical and simulation models as an alternative to cadavers, presenting a valuable option for initial clinical practice preceding engagement with live animals. Some of the advantages of 3D printed models include increased durability, low production costs, and a reduction in the number of cadavers used in teaching. AcknowledgmentsThe authors thank all the students who participated in this study. Conflict of interestThe authors declare no conflict of interest. FundingThis research was supported by a grant from the Sarajevo Canton Ministry for Sciences, Higher Education and Youth for 2023 (project number 27-02-35-37080-13/23). Authors’ contributionsNH and AŠR conceived and designed the study. Data entry, analysis, and interpretation: AŠR, AM, and LŠ. The manuscript was drafted by NH and FT, and LŠ and AM revised the intellectual content. All authors have read, reviewed, and approved the final version of the manuscript. Data availabilityThe data supporting the findings of this study are available from the corresponding author upon reasonable request. ReferencesAl-Elq, A.H. 2010. Simulation-based medical teaching and learning. J. Fam. Comm. Med. 17(1), 35–40. Altwal, J., Wilson, C.H. and Griffon, D.J. 2022. Applications of 3-dimensional printing in small-animal surgery: a review of current practices. Vet. Surg. 51(1), 34–51. Baillie, S. 2007. Utilisation of simulators in veterinary training. Cattle Pract. 15(3), 224–228. Braid, H.R. 2022. The use of simulators for teaching practical clinical skills to veterinary students — a review. Altern. Lab. Anim. 50(3), 184–194. Casimir, R., Linn, L., King, H., McKenzie, D., Thompson, M. and Perry, R. L. 2022. Simulation models: another approach to teaching and learning. J. Am. Vet. Med. Assoc. 261(1), 47. Chedid, V.G., Kamath, A.A., Knudsen, J., Frimannsdottir, K., Yost, K.J., Geske, J., Morris, J.M., Taner, T., Matsumoto, J.M. and Kamath, P.S. 2020. Three-dimensional-printed liver model helps learners identify hepatic subsegments: a randomized-controlled cross-over trial. Am. J. Gastroenterol. 115(11), 1906–1910. Chen, Y., Qian, C., Shen, R., Wu, D., Bian, L., Qu, H., Fan, X., Liu, Z., Li, Y. and Xia, J. 2020. 3D printing technology improves medical interns’ understanding of anatomy of gastrocolic trunk. J. Surg. Educ. 77(5), 1279–1284. Cheo, F.Y., Soeharno, H. and Woo, Y.L. 2024. Cost-effective office 3D printing process in orthopaedics and its benefits: a case presentation and literature review. Proc. Singapore Healthcare, 33, 1–7. Cojocaru, V., Frunzaverde, D., Miclosina, C.O. and Marginean, G. 2022. The influence of the process parameters on the mechanical properties of PLA specimens produced by fused filament fabrication-a review. Polymers 14(5), 886. Díaz-Regañón, D., Mendaza-De Cal, R., García-Sancho, M., Rodríguez-Franco, F., Sainz, Á., Rodriguez-Quiros, J. and Rojo, C. 2024. Canine upper digestive tract 3D model: assessing its utility for anatomy and upper endoscopy learning. Animals, 14(7), 1070. Ekim, O., Bakici, C., Akçay, A., Algin, O. and Oto, C. 2024. The efficiency of 3D-printed dog brain ventricular models from 3 tesla (3T) magnetic resonance imaging (MRI) for neuroanatomy education. Pak. Vet. J. 44(2), 430–436. Erickson, T.K. 2019. Stress in the veterinary medical field: a literature review, Northern Illinois University, US. Honors Capstones, pp 1052. Fredieu, J.R., Kerbo, J., Herron, M., Klatte, R. and Cooke, M. 2015. Anatomical models: a digital revolution. Med. Sci. Educ. 25, 183–194. Griffey, J. 2014. The types of 3-D printing. Library Tech. Rep. 50(5), 8–12. Hadžiomerović, N., Hadžiomerović, A.I., Avdić, R., Muminović, A., Tandir, F., Bejdić, P. and Pandžić, A. 2023. Students’ performance in teaching neuroanatomy using traditional and technology-based methods. Anat. Histol. Embryol. 52(1), 115–122. Hammerton, C., Yip, S.W.L., Manobharath, N., Myers, G. and Sturrock, A. 2022. Are 3D printed models acceptable in assessment? Clin. Teacher 19(3), 221–228. Issenberg, S.B., McGaghie, W.C., Petrusa, E.R., Lee Gordon, D. and Scalese, R.J. 2005. Features and uses of high-fidelity medical simulations that lead to effective learning: a BEME systematic review. Med. Teacher 27(1), 10–28. Kapoor, K. 2024. 3D visualization and printing: an “anatomical engineering” trend revealing underlying morphology via innovation and reconstruction towards future of veterinary anatomy. Anat. Sci. Int. 99(1), 159–182. Kurt, S., Selviler-Sizer, S., Onuk, B. and Kabak, M. 2022. Comparison of sheep scapula models created with polylactic acid and thermoplastic polyurethane filaments by three-dimensional modelling. Anat. Histol. Embryol. 51(2), 244–249. Langebæk, R., Eika, B., Jensen, A.L., Tanggaard, L., Toft, N. and Berendt, M. 2012. Anxiety in veterinary surgical students: a quantitative study. J. Vet. Med. Educ. 39(4), 331–340. Leukers, B., Gülkan, H., Irsen, S.H., Milz, S., Tille, C., Schieker, M. and Seitz, H. 2005. Hydroxyapatite scaffolds for bone tissue engineering made by 3D printing. J. Mater. Sci. Mater. Med. 16(12), 1121–1124. Marsch, S., Yanagida, T. and Steinberg, E. 2024. Stressors and stress of veterinary students during their Introduction to the clinical workplace. J. Vet. Med Educ. 52(1):139–151. Mendaza-De Cal, R.M. and Rojo, C. 2021. 3D-printed model of the ovine stomach by surface scanning: evaluation for teaching veterinary anatomy. Int. J. Morphol. 39(5), 1480–1486. Neubauer, V., Gächter, A., Probst, T., Brühl, D., Dale, R., Pieh, C. and Humer, E. 2024. Stress factors in veterinary medicine - a cross-sectional study among veterinary students and practicing vets in Austria. Front. Vet. Sci. 1389042. O’Brien, C., Souza, C. A., Sheikh, A., Miguel, O. and Wood, T. 2021. Use of tracheobronchial tree 3-dimensional printed model: does it improve trainees’ understanding of segmentation anatomy? A prospective study. 3D Print. Med. 7(1), 2. Perez-Rivero, J. J., and Rendon-Franco, E. 2012. Experience of the use of table-top simulators as alternatives in the primary surgical training of veterinary undergraduate students. Altern. Lab. Anim. 40(5), 10–11. Pohl, R., Botscharow, J., Böckelmann, I. and Thielmann, B. 2022. Stress and strain among veterinarians: a scoping review. Irish Vet. J. 75(1), 15. Rengier, F., Mehndiratta, A., von Tengg-Kobligk, H., Zechmann, C. M., Unterhinninghofen, R., Kauczor, H.-U. and Giese, F.L. 2010. 3D printing based on imaging data: review of medical applications. Int. J. Comput. Ass. Rad. 5, 335–341. Scalese, R.J. and Issenberg, S.B. 2005. Effective use of simulations for the teaching and acquisition of veterinary professional and clinical skills. J. Vet. Med. Educ. 32(4), 461–467. Thompson, J.L., MacKay, J. and Bowlt Blacklock, K. 2023. Evaluation of veterinary students’ confidence and competence with surgical entrustable professional activities after repeated use of low-fidelity training models. Vet. Rec. 192(8), e2779. Wang, Z., Liu, Y., Luo, H., Gao, C., Zhang, J. and Dai, Y. 2017. Is a three-dimensional printing model better than a traditional cardiac model for medical education? A pilot randomized controlled study. Acta Cardiol. Sin. 33(6), 664–669. Wilhite, R. and Wölfel, I. 2019. 3D printing for veterinary anatomy: an overview. Anat. Histol. Embryol. 48(6), 609–620. Yilgör Huri, P. and Oto, Ç. 2022. 3D printing in veterinary medicine. Ankara Univ. Vet. Fak. 69, 111–117. | ||
| How to Cite this Article |
| Pubmed Style Hadžiomerović N, Šunje-rizvan A, Maksimović A, Šatrović L, Tandir F. Use of 3D printed low-cost models for veterinary clinical skills training. Open Vet. J.. 2025; 15(2): 863-870. doi:10.5455/OVJ.2025.v15.i2.35 Web Style Hadžiomerović N, Šunje-rizvan A, Maksimović A, Šatrović L, Tandir F. Use of 3D printed low-cost models for veterinary clinical skills training. https://www.openveterinaryjournal.com/?mno=228541 [Access: January 25, 2026]. doi:10.5455/OVJ.2025.v15.i2.35 AMA (American Medical Association) Style Hadžiomerović N, Šunje-rizvan A, Maksimović A, Šatrović L, Tandir F. Use of 3D printed low-cost models for veterinary clinical skills training. Open Vet. J.. 2025; 15(2): 863-870. doi:10.5455/OVJ.2025.v15.i2.35 Vancouver/ICMJE Style Hadžiomerović N, Šunje-rizvan A, Maksimović A, Šatrović L, Tandir F. Use of 3D printed low-cost models for veterinary clinical skills training. Open Vet. J.. (2025), [cited January 25, 2026]; 15(2): 863-870. doi:10.5455/OVJ.2025.v15.i2.35 Harvard Style Hadžiomerović, N., Šunje-rizvan, . A., Maksimović, . A., Šatrović, . L. & Tandir, . F. (2025) Use of 3D printed low-cost models for veterinary clinical skills training. Open Vet. J., 15 (2), 863-870. doi:10.5455/OVJ.2025.v15.i2.35 Turabian Style Hadžiomerović, Nedžad, Amila Šunje-rizvan, Alan Maksimović, Lejla Šatrović, and Faruk Tandir. 2025. Use of 3D printed low-cost models for veterinary clinical skills training. Open Veterinary Journal, 15 (2), 863-870. doi:10.5455/OVJ.2025.v15.i2.35 Chicago Style Hadžiomerović, Nedžad, Amila Šunje-rizvan, Alan Maksimović, Lejla Šatrović, and Faruk Tandir. "Use of 3D printed low-cost models for veterinary clinical skills training." Open Veterinary Journal 15 (2025), 863-870. doi:10.5455/OVJ.2025.v15.i2.35 MLA (The Modern Language Association) Style Hadžiomerović, Nedžad, Amila Šunje-rizvan, Alan Maksimović, Lejla Šatrović, and Faruk Tandir. "Use of 3D printed low-cost models for veterinary clinical skills training." Open Veterinary Journal 15.2 (2025), 863-870. Print. doi:10.5455/OVJ.2025.v15.i2.35 APA (American Psychological Association) Style Hadžiomerović, N., Šunje-rizvan, . A., Maksimović, . A., Šatrović, . L. & Tandir, . F. (2025) Use of 3D printed low-cost models for veterinary clinical skills training. Open Veterinary Journal, 15 (2), 863-870. doi:10.5455/OVJ.2025.v15.i2.35 |